A huge amount of work has taken place to help the health board face the unprecedented challenges posed by the Coronavirus pandemic.
The number of confirmed new cases rose by 180 today in Wales, bringing the total number of confirmed cases to 921.
There has also been six further deaths of people who had tested positive for Novel Coronavirus (COVID-19). The total number of deaths in Wales is now 34.
There have been sweeping changes across hospitals, while staff have taken on extra duties, additional training and even different roles to ensure the best possible patient care is provided.
Everyone from health board executives and senior managers, frontline staff and support teams – in hospitals, in the community and elsewhere –are involved in this never-before-seen effort.
Swansea Bay’s Chief Executive Tracy Myhill said:
“So much has changed over recent weeks. The scale and pace of the range of actions is difficult to appreciate.
“Our first wave of preparation has gone very well.
“It’s remarkable where we have got to in such a short time and I appreciate the ongoing work to enable us to be as prepared as we can be for what’s coming.”
Most outpatient clinics have been suspended and non-emergency surgical work postponed. This was necessary to reprioritise how staff and resources are used to keep patients safe.
In Morriston Hospital, the Surgical Decision Making Unit (SDMU) and Surgical Short Stay Unit (SSSU) have moved to what was the fracture clinic in the main outpatients building.
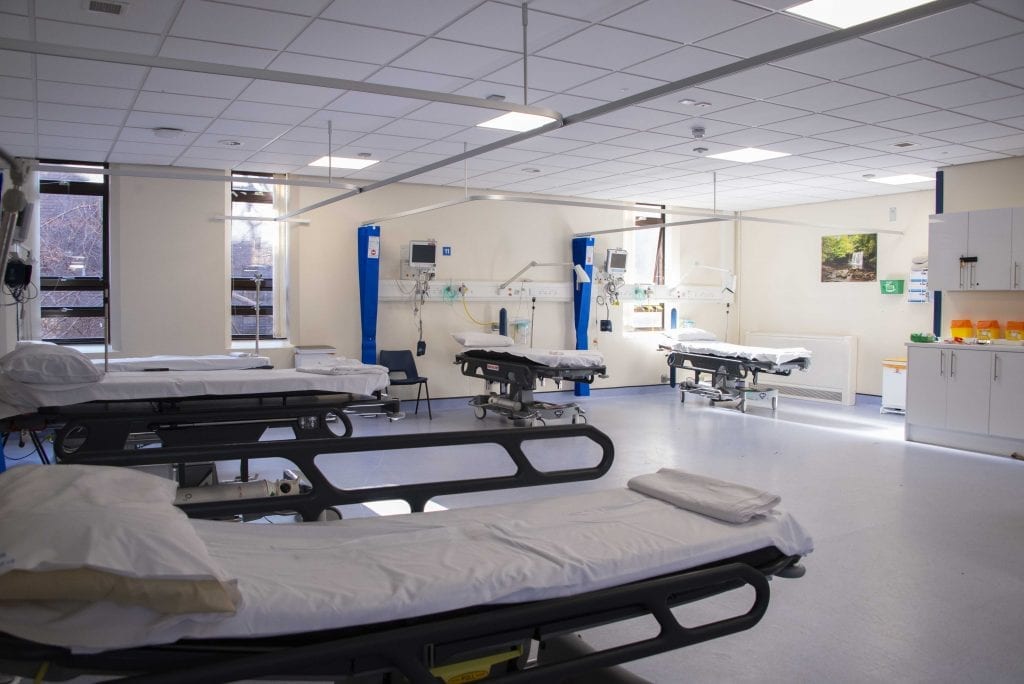

A Respiratory Assessment Unit (RAU) has now been established in the former Surgical Decision Making Unit area. It has a separate entrance providing direct access for patients brought in by ambulance.
Morriston Hospital director Deb Lewis said: “We have been working with our ambulance service colleagues to develop new pathways that can take patients directly to the RAU.
“If they are suspected COVID but no other illness or injury they will go to the RAU.
“If they have a primary illness or injury that requires the input of Emergency Department (ED) clinicians then patients will go to the ED irrespective of any Coronavirus symptoms.
“Any of these patients with Coronavirus symptoms will be managed in designated areas within the ED.”
Not all patients arriving at the RAU will need hospital admission. Even if testing shows they have Coronavirus, many will be able to go home and follow the established isolation rules.
Mrs Lewis said: “There is also an ambulatory area where they may need to stay for a few hours for oxygen or further tests.
“There are also 12 beds for patients who need more support and may need onward admission to the main wards. If they need immediate ventilation they will go straight to critical care.”
In the coming weeks demand for critical care is expected to rise, with a high percentage of patients requiring the use of a ventilator.
Morriston has the capacity to expand to provide 93 critical care beds for very sick patients who need ventilation.
However, this requires six nurses for every patient for 24/7 cover. So if all 93 beds had to be deployed, this would require almost 600 staff.
Postponing most surgery has released theatre staff to undergo special training to manage ventilated patients. Training is provided in-house, in association with Swansea University.
Of course, patients are still arriving at the hospital’s Emergency Department with a wide range of illnesses or injuries – including those triaged on ambulances and suspected to have Coronavirus.


Mrs Lewis said: “We have split ED into two areas: red for Coronavirus and blue for non-Coronavirus. Each has its own triage, resuscitation and treatment areas.
“So if a patient comes in with an illness or injury but has Coronavirus symptoms, they go to red. If they don’t have symptoms they go to blue.
“We are also opening an ambulance decontamination unit on-site. Ambulances bringing suspected Coronavirus patients in have to be decontaminated at a location off-site, some distance away.
“This could mean vehicles are off-road for a long time so we have worked with the ambulance service to put one here.”
Additional facilities have also been introduced for staff, including 24 new shower units and six sinks to help with hand hygiene.


Meanwhile, the Morriston fracture clinic has moved a short distance away within the outpatient department, and is now also the temporary home of the Minor Injury Unit which has relocated from near the ED.
“Our orthopaedic consultants have taken on responsibility for the MIU, and are providing additional support in the MIU in Neath Port Talbot,” said Mrs Lewis.
“They can manage a greater acuity of patients, which will reduce the number of patients having to be seen in Morriston ED.”
Other changes include creating a dedicated new entrance for paediatric patients at the pharmacy end of the main corridor. Children will be seen in the former SSSU, except those with minor injuries who go to the MIU.
Mrs Lewis paid tribute to staff, saying: “They’ve been incredible from day one and I can’t thank them enough. We’ve moved mountains this week”.








Leave a Reply
View Comments